Dr. Bhagwati Wadwekar, W09478
Abstract
Purpose:This study aims to analyze the impact of complete excision of posterior remnant tissue(ExPRT) on outcome of modified single anterior flap external dacryocystorhinostomy(mSAF-EDCR).
Methods:We analysed records of all patients of primary acquired nasolacrimal duct obstruction (PANDO) who had undergone mSAF-EDCR with complete ExPRT between August 2014 and October 2016. We analysed operative time, complications and surgical outcome of these patients.
Results:Forty-one patients had undergone mSAF-EDCR with complete ExPRT. Average surgical time was 36 minutes (range 28 to 50). The most common complications were intraoperative bleeding in four cases and torn sac flap in two cases. laceration of nasal mucosa in one case and extension of skin incision in one case. Follow-up was done at tenth day and one month post-operatively. There was complete absence of watering in 36 patients and occasional watering in five patients. Tear meniscus height was normal for all patients. Syringing was patent in all 41(100%) patients. Hence both subjective and objective success rates were 100%.
Conclusion:Our series of cases mSAF-EDCR demonstrated 100% success rate which may be attributed to complete ExPRT. Our study also indicates that mSAF-EDCR is technically easier and time saving, and should be preferred over conventional EDCR . The complications related to flap damage are also more easily manageable in mSAF-EDCR than conventional EDCR. These results also prompt future research to assess complete ExPRT during mSAF-EDCR surgery.
Keywords:
Dacryocystitis, lacrimal, epiphora, dacryocystorhinostomy, nasolacrimal duct obstruction, mucosal flap
Introduction
Conventional external dacryocystorhinostomy (EDCR) is done by giving H shaped incision on lacrimal sac and nasal mucosa, thus making anterior and posterior flaps of these structures. The anterior lacrimal sac flap (ALSF) is then sutured with anterior nasal mucosa flap (ANMF) and the posterior lacrimal sac flap (PLSF) is sutured with posterior nasal mucosa flap (PNMF), thus making a channel that bypasses naso-lacrimal duct.1, 2 Making all the four flaps and suturing of flaps together is technically challenging and time-consuming, more so in difficult cases and in cases with excessive intra-operative bleeding.[3, 4, 5, 6,7,8,9]
EDCR has evolved in many ways over a period. While doing conventional EDCR, it is difficult to suture PLSF to PNMF because of the depth and narrow surgical space. To overcome this difficulty some surgeons suture only anterior flaps, excising or leaving behind posterior flaps as such.[3,4,5,6,7] Further studies have shown that the procedure can even be done by making single large anterior flaps of sac and nasal mucosa, andsuturing them without making posterior flaps at all. This makes the procedure easier and less time consuming.[10,11,12] This modified single large anterior flap EDCR (mSAF-EDCR) was first devised by Baldeschi L et al. We also prefer to use mSAF-EDCRin our patients but in addition to the usual steps of this procedure we also excise every bit of the posterior remnant tissue of sac and nasal mucosa. We believe that complete excision of posterior remnant tissue (ExPRT) of sac and nasal mucosa may reduce complications like common canalicular obstruction and sump like syndrome, and thus improve the success rate of this procedure.Complete ExPRT during mSAF-EDCRhas not been studied till now.
The primary goal of present study is to analyze the impact of completeExPRT on outcome of mSAF-EDCR. The secondary goal is to measure surgical time and study complications of this procedure.
Materials and Methods
We retrieved and analyzed the records of all patients of primary acquired nasolacrimal duct obstruction (PANDO) who had undergone mSAF-EDCR with complete ExPRT between August 2014 and October 2016. Ethics approval was taken from the Institutional Ethics Committee and study was conducted in accordance of the Declaration of Helsinki.Patients with incomplete records, age less than 16years, secondary acquired nasolacrimal duct obstruction, canalicular /common canalicular obstruction, and chronic dacryocystitis with fistula were excluded. We recorded the demographics, pre-operative assessment, operative details, post-operative management and clinical outcomes. We analyzed the clinical outcomes of surgery both subjectively and objectively. Absent or occasionalpost-operative watering were considered subjective success, whereas patent syringing at the end of 1 month of surgery was considered objective success. We recorded presence ofpersistent watering, non-patent and partially patent syringing as surgical failure. Operative time, complications and follow up details were also noted.
Results
Records revealed that we had performed mSAF-EDCR with complete ExPRT in 51 PANDO patients. We excluded cases with incomplete records (4 cases), age < 16 years (2 cases), secondary acquired nasolacrimal duct obstruction (2 cases), canalicular /common canalicular obstruction(1 case), and chronic dacryocystitis with fistula(1 case). Forty-one patients who had undergone mSAF-EDCR with complete ExPRTwere analyzed. Nineteen(46.34%) patients were females and twenty-two(53.65%) were males. Mean age of patients was 56.43 years ( range 29to 80). The demographics of these patients are given in table 1.
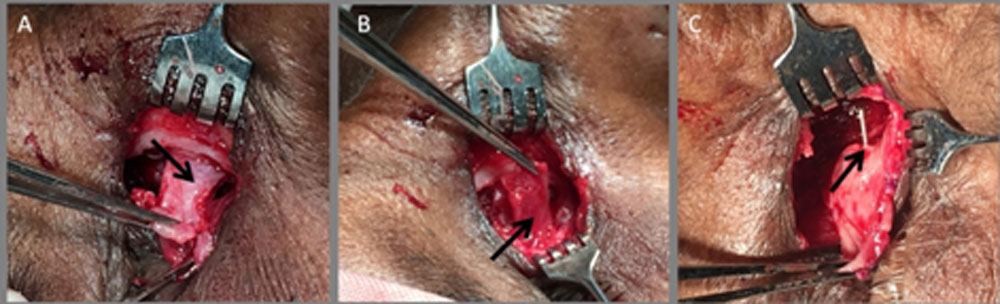
All surgeries were done by single oculoplastic surgeon (BW). Tissue was infiltrated by giving local anaesthesia which consisted of an equal mixture of 2% lignocaine and 0.5% bupivacaine, with 1:100,000 adrenaline. Sixmillilitreswas injected overlacrimal crest, 2ml in the infratrochlear region and 2ml in the infraorbital region.The nasal packing was done with gauze soaked in 4%lignocaine and 1:100,000 adrenaline. Skin and muscle were retracted after making 10mm curvilinear tear trough incision. The sac was identified and reflected laterally. The periosteum was vertically incised anterior to the lacrimal crest and elevated from the lacrimal fossa using Freer’s elevator. A bony ostium 15mm x 15mm was made with Kerrison’s punch. The largest possible single U shaped flap ofnasal mucosa was made (figure A). Similarly, largest possible U shaped flap oflacrimal sac mucosa was made with 11number Bard-Parker’s knife after tenting sac with Bowman’s probe (figure B). The remnant posterior sac tissue especially posterior to common canalicular opening was completely excised. Bowman’s probe was passed from the lower punctum through the canaliculus and its smooth free passage through the common canalicular opening was confirmed by passing probe few times (figure C). Any tissue obstructing the free passage at the common canalicular opening was excised. Posterior remnant nasal mucosa was also completely excised. Anteriorflaps were trimmed if they were very large. The anterior flap of the sac was sutured to the anterior flap of the nasal mucosa with three interrupted 6-0 vicryl sutures to prevent sagging under tension. The orbicularis muscle and skin were closed with interrupted 6-0 vicryl sutures at the end of the procedure. Syringing was done to ensure the patency. Average time required to complete the surgery was 36 minutes (range 28 to 50 minutes). Complications consisted of intraoperative bleeding in four cases, torn sac flap in two cases, laceration of nasal mucosa in one case and extension of skin incision in one case. Postoperatively tablet ciprofloxacin 500 mg and serratiopeptidase( 10mg) and diclofenac (50 mg) tablet were given twice daily for five to seven days to all patients.Nasal decongestantoxymetazoline (0.5 mg/ml) was administered as one drop four times dailyon the side of surgery for one week. Ciprofloxacin (0.03mg/10ml) and dexamethasone (0.01mg/10ml) eye-drops were instilled four times dailyfor the first week post-operatively on the side of surgery which were tapered and stopped over one month. Nose pack was removedand syringing was done for all the patients on 1st post-operative day. All patients were discharged on second post-operative day.
Follow-up was doneon tenth day and at one month post-operatively. Syringing was done attenth postoperative day and at one month follow-up whereas fluorescein dye disappearance test was done at one month follow-up.
There was complete absence of watering at follow-ups in 36 patients. Five patients had occasional watering on tenth day and at one month post-operatively. Tear meniscus height was normal for all patients at the end of one month. Syringing was patent in all 41(100%) patients at the end of surgery and remained patent on subsequent follow-ups. Hence both subjective and objective success rates were 100%. One case developed suture abscess on 10th post-operative day. Thefluorescein dye disappearance test (FDDT) was < 5 minutes in all patients. Follow up findings and outcomes are given in table 2.
Discussion
Allof our patients underwent mSAF-EDCRwith complete ExPRT. We could achieve subjective and objective success rate of 100%. The average surgical time taken for our procedure was 36 min. Nine of our patients developed complications.
Conventional EDCR is difficult to perform and requires considerable operative time. Various modifications of conventional EDCR have been suggested by surgeons to make it easier, less time consuming and improve its outcome (table 3). The conventional EDCR is done by making anterior and posterior flaps, and subsequently suturing them.Baldeschi L et al, Tetikoglu M et al and Caglar C et al modified this technique and recommended doing EDCR by making onlysingle large anterior flaps. They stressed the point that this surgery can be done without making posterior flaps andthis modification does not affect the success rate. These recent studiesrecommend anterior flap only technique for all EDCR surgeries.We also followedthis modified techniquein all our patients.However our surgical technique differed in two ways. Firstly, these studies mention suspension of sutured bridge to overlying orbicularis to prevent sagging of flap, which improves clinical outcome and success rate. [10, 11, 12] In our patients we had achieved same result by trimming both the flaps to make them taught. Secondly, we also performed complete ExPRT.It has been recommended that in EDCR surgeries (conventional and modified) which involve making posterior flaps, excising or suturing them reduces chances of post-operative obstruction. Although posterior flaps are not formed in mSAF-EDCR, we have observed that even after making a large single anterior flap of sac and nasal mucosa, some remnant tissue of sac flap and posterior nasal mucosa is invariably left behind. Going by general surgical principles, any remanant tissue has potential for granuloma formation and scarring. Thus posterior remnant sac tissue may cause common canalicular obstruction especially if it is left behind common canalicular opening.On the other hand remnant posterior nasal mucosa may cause sump syndrome like symptoms.[13] Hence we need to excise these structures completely. In their case report, Sodhi PK et al concluded that single large anterior nasal and lacrimal mucosal flaps should be preferred over double flaps. They also reinforced that additional removal of every bit of remnant of posterior nasal flap may prevent sump syndrome. However, in study by khan et al common canalicular duct obstruction occurred in two cases in spite of posterior flaps excision. They could not find any reason but it might have been due to incomplete ExPRT.[14]Study by Tetikoglu M et al is the only other study that mentions excision of PLSF and PNMF in mSAF-EDCR but they did not mention complete ExPRT.[12] In fact we did not find any study that has discussed complete ExPRT during mSAF-EDCR.
Previous studies have reported success rate of 73% to 97.6% in conventional EDCR, 79% to 96.7% in modified EDCR and 94.9% to 100% in mSAF-EDCR. We achieved 100% subjective and objective success rate in our patients. The only other study to have achieved 100% success rate till date was done by Baldeschi L et al in 2004whohad also performed mSAF-EDCR. However, it must be noted that the group in which mSAF-EDCR was performed comprised of only twentynine patients.[15]One of the previous study by same author, which was also the first study to describe mSAF-EDCR, had higher failure rate, with seven out of 45 patients (16%) requiring probing in initial post-operative period.[10]However, these patients did not have tearing at 17 months follow-up.Many studies have compared outcomes of conventional EDCR and modified EDCR (table 4) but there is only one study that has compared outcomes of conventional EDCR andmSAF-EDCR.[15]The differences in outcomes of conventional, modified EDCR and mSAF-EDCR are not statistically significant and these procedures have no advantage over each other as far as outcomes are concerned but later two have benefits of ease of procedure and reduced surgical time. Meta-analyses of seven studies by Bukhari et al analysing 765 eyes also reached the same conclusion.[16]
The mean surgical time in our study was 36 min (range, 28 to 50). Operative time was in the higher (mean: 47 min) in four of our cases who had excessive bleeding during the procedure. Mean operative times reported in literature for conventional EDCR varies from 45-90 minutes[17,18,19]34-36 min for modified EDCR[6,8] and 28-34 min for m-SAF-EDCR.[10,12]Most studies demonstrate that modified EDCR is much less time consuming than conventional EDCR. The average time taken to complete the procedure in our study was also much lesser than time taken to perform conventional EDCR in previous studies. In addition to usual steps of mSAF-EDCR we had also performed complete ExPRT and hence we expected that this step would add to our surgical time. But we found that our meansurgical time was similar to meansurgical time of other studies in whichmodified EDCR was done. We also compared our mean surgical time with the time taken to perform mSAF-DCR without complete ExPRT in previous studies. Apart from lesser mean surgical time taken byBaldeschi et al (28 min) our mean surgical time was similar to that of others. Surgical time and outcomes of mSAF-EDCR have been summerised in table 5.
Surgery was uneventful in thirty-two cases. Complications occurred in nine (21.95%) of our cases. Most common intraoperative complication in our cases was bleeding which occurred in four cases ( 9.75%). The reported incidence of this complication in previous studies varies from (5.3 to 12%).The double-flap technique of conventional EDCR is expected to reduce the possibility of intraoperative bleeding. Serin D et al and Katuwal S et al studied this aspect and found thatthere is no significant difference between postoperative bleeding scores of conventional and modified EDCR patients.The other complications comprised of torn sac flap in two cases (4.87%), laceration of nasal mucosa in one(2.83%), extension of skin incision in one(2.83%), and suture abscess in one (2.83%).Two of the cases had small and fibrosed lacrimal sac. This resulted in small ALSF formation, ultimately leading to its tearing during surgery. We could still easily approximate remaining part of ALSF to ANMF because of large size of ANMF. This would not have been possible in conventional EDCR because of smaller flap size. Similarly in case of lacerated ANMF we could suture both flaps because of availability of large ALSF. Hence in addition to being technically easier and less time consuming, than conventional EDCR complications like torn flaps are more easily manageable in mSAF-EDCR due to large size of flaps.
All patients had patent syringing immediate post-operative, one day later and at one month follow up. Five patients had occasional watering. All of them were more than 70 years of age.Their FDDT done at one month ranged more than 2 minutes, indicating lacrimal pump failure as possible cause for watering.
We acknowledge that there were few limitations in our study. Our study had retrospective design. However this factor is partially mitigated bythe fact that this is a single centre study and all the surgeries were done by single surgeon (BW) who also maintained the records. We also did not find any patients inwhom complete ExPRT was not performed.Hence comparative analysis could not be done.
We recommend that prospective case control study should be performed to analyse complete ExPRT during mSAF-EDCR surgery to establish higher level of evidence.
Conclusion
Our series of cases mSAF-EDCR demonstrated 100% success rate which may be attributed to complete ExPRT. Our study also indicates that mSAF-EDCR is technically easier and time saving, and should be preferred over conventional EDCR . The complications related to flap damage are also more easily manageable in mSAF-EDCR than conventional EDCR. These results also prompt future research to assess complete ExPRT during mSAF-EDCR surgery.
Declaration Of Interest
The author reports no conflict of interest. The author alone is responsible for thecontent and writing of the paper.
References
- Ali MJ, Naik MN, Honavar SG. External dacryocystorhinostomy: Tips and tricks. Oman journal of ophthalmology. 2012;5(3):191.Deshpande S, Agashe A, Loomba A, Dhiware N. Step-by-step dacryocystorhinostomy for beginners: An expert’s view. Journal of Clinical Ophthalmology and Research. 2014;2(3):161.
- Serin D, Alagöz G, Karsloglu S, Çelebi S, Kükner S. External dacryocystorhinostomy: double-flap anastomosis or excision of the posterior flaps?.Ophthalmic Plastic & Reconstructive Surgery. 2007;23(1):28-31.
- Türkcü FM, Öner V, Taş M, Alakuş F, İşcan Y. Anastomosis of both posterior and anterior flaps or only anterior flaps in external dacryocystorhinostomy. Orbit. 2012;31(6):383-5.
- Katuwal S, Aujla JS, Limbu B, Saiju R, Ruit S. External dacryocystorhinostomy: do we really need to repair the posterior flap?.Orbit. 2013;32(2):102-6.
- Kacaniku G, Begolli I. External dacryocystorhinostomy with and without suturing the posterior mucosal flaps. Medical Archives. 2014;68(1):54.
- Elwan S. A randomized study comparing DCR with and without excision of the posterior mucosal flap. Orbit. 2003;22(1):7-13.
- Sharma HR, Sharma AK, Sharma R. Modified External Dacryocystorhinostomy in Primary Acquired Nasolacrimal Duct Obstruction. Journal of clinical and diagnostic research. 2015;9(10).doi: 10.7860/JCDR/2015/15940.6624
- Pandya VB, Lee S, Benger R, Danks JJ, Kourt G, Martin PA et al. The role of mucosal flaps in external dacryocystorhinostomy. Orbit. 2010 Dec 1;29(6):324-7.
- Baldeschi L, Nardi M, Hintschich CR, Koornneef L. Anterior suspended flaps: a modified approach for external dacryocystorhinostomy. British journal of ophthalmology. 1998;82(7):790-2.
- Caglar C, Yener HI, Gul A, Ozcimen M. The Modified Technique of External Dacryocystorhinostomy in the Management of Complicated Nasolacrimal Duct Obstruction. Journal of Craniofacial Surgery. 2016;27(2):416-9.
- Tetikoglu M, Sagdik HM, Ozcura F, Aktas S. Assessment of anterior suspended flaps modification for external dacryocystorhinostomy. Journal of Craniofacial Surgery. 2015;26(3):789-91.
- Sodhi PK, Verma L, Ratan SK. Transient recurrence of pressure regurgitation following successful conventional external dacryocystorhinostomy. Journal of Cranio-Maxillofacial Surgery. 2005;33(3):210-1.
- Khan FA, Yaqub MA, Fayyaz M. The importance of excising or suturing the posterior mucosal flaps in external dacryocystorhinostomy. Pak J Ophthalmol. 2010;26(2):69-73.
- Baldeschi L, MacAndie K, Hintschich CR. The length of unsutured mucosal margins in external dacryocystorhinostomy. American journal of ophthalmology. 2004;138(5):840-4.
- Bukhari AA. Meta-analysis of the effect of posterior mucosal flap anastomosis in primary external dacryocystorhinostomy. Clinical ophthalmology (Auckland, NZ). 2013;7:2281.
- Zaman M, Babar TF, Abdullah A. Prospective randomized comparison of dacryocystorhinostomy (DCR) with and without intubation. Pak J Med Res. 2005;44(2):75-8.
- Hartikainen J, Antila J, Varpula M, Puukka P. Prospective randomized comparison of endonasal endoscopic dacryocystorhinostomy and external dacryocystorhinostomy. Laryngoscope.1998;108:1861–1866.
- Uludag G, Yeniad B, Ceylan E, Yildiz-Tas A, Kozer-Bilgin L. Outcome comparison between transcanalicular and external dacryocystorhinostomy. Int J Ophthalmol. 2015;8:353-57.
Table 1.Demographic profile of study population
| Characteristic | Number of patients(N) | Percentage (%) |
| Total number of patients | 41 | 100 |
| Age group in years | ||
| 20-40 | 9 | 21.95 |
| 41-60 | 17 | 41.46 |
| >60 | 15 | 36.58 |
| Sex | ||
| Male | 21 | 51.21 |
| Female | 20 | 48.78 |
| Eye Affected | ||
| Right | 19 | 46.34 |
| Left | 22 | 53.65 |
Table 2. Postoperative follow-up and outcomes at 1 month
| Characteristics | Number of Patients | Percentage of total (N=41) |
| Symptoms | ||
| No Watering | 36 | 87.8 |
| Occasional Watering | 5 | 12.2 |
| Watering | 0 | 0 |
| Results of Syringing | ||
| Patent | 41 | 100 |
| Partially Patent | 0 | 0 |
| Non patent | 0 | 0 |
| Fluorescein Dye Disappearance test(FDDT) | ||
| < 2 minutes | 36 | 87.5 |
| 2 to 5minutes | 5 | 12.2 |
| >5 minutes | 0 | 0 |
| Success Rate | ||
| Objective(Patent Syringing) | 41 | 100 |
| Subjective(Symptom free) | 41 | 100 |
Table 3. Modifications of EDCR
| EDCR types | Incision shape | Flaps made | Structures sutured | Flaps and Structures Excised | |||||
| ANMF | ALSF | PNMF | PLSF | ANMF to ALSF |
PNMF to PLSF |
||||
| 1 | Conventional | H | Yes | Yes | Yes | Yes | Yes | Yes | None |
| 2 | Modified | H | Yes | Yes | Yes | Yes | Yes | No | None (Posterior flaps left behind not excised) |
| 3 | Modified | H | Yes | Yes | Yes | Yes | Yes | No | Posterior flaps |
| 4 | Modified | U | Single large | Single large | Not made | Not made | Yes | No | No excision |
| 5 | Present study | U | Single large | Single large | Not made | Not made | Yes | No | Every bit of posterior remnant sac and nasal mucosa tissue |
EDCR:External dacryocystorhinostomy,ANMF: Anterior nasal mucosa flap, ALSF: Anterior lacrimal sac flap, PNMF:Posterior nasal mucosa flap, PLSF: Posterior lacrimal sac flap
Table 4.Comparisionof success rates: Conventional EDCR VS modified EDCR
| Success rate (%) | ||
| Conventional EDCR | Modified EDCR | |
| Dareshani et al, 1996 | 97.6 | 94.2 |
| Elwan S et al 2003 | 85 | 90 |
| Serin D et al 2007 | 93.75 | 96.67 |
| Pandya V et al, 2010 | 73 | 79 |
| Khan FA et al2010 | 97.1 | 94.3 |
| Turkcu FM et al. 2011 | 89.8 | 89.4 |
| Katuwal S et al. 2013 | 90.7 | 87.5 |
| Kacaniku G. et al. 2014 | 95.3 | 96.2 |
EDCR (external dacryocystorhinostomy)
Table 5.Modified single large anterior flap only EDCR (mSAF-EDCR): Outcomes and mean surgical time
| Study | Number of eyes (n) | Success rate(%) | MeanSurgical time in minutes |
| Baldeschi et al 2004 | 29 | 100 | 28.6 |
| Tetikoglu M et al 2015 | 50 | 96 | 34 |
| Caglar C et al 2016 | 118 | 94.9 | NA |
| Our Study | 41 | 100 | 36 |
NA: not available
Figure A: Large nasal mucosal flap
Figure B: Large lacrimal sac flap
Figure C: Confirming free pass of Bowman’s probe



Leave a Comment