Dr Priyanka V Walvekar, P20976,Dr Chinmayee Thrishula Murthy, Dr Sri Ganesh
ABSTRACT:
Title: Efficacy of Perforated Punctal Plugs in unilateral/bilateral punctal stenosis with ocular allergy
Aim: To report the efficacy, tolerance and initial clinical outcome of implanted perforated punctual plugs in cases of unilateral/ bilateral punctual stenosis due to long standing ocular allergy.
Materials and methods: Eleven eyes with punctal stenosis secondary to ocular allergy who received perforated punctal plug implants were included. Epiphora scoring, biomicroscopic examination, fluorescein dye disappearance test [FDDT], punctal dilatation, canaliculi probing & nasolacrimal duct irrigation assessed. Biomicroscopic examination, FDDT and plug tolerance were documented at postoperative 1st day, 1st M & 3rd M.
Results: Free passage into the nose obtained with nasolacrimal system irrigation. Fluorescein dye disappearance test post implantation found to be under 3 minutes in all.
Conclusion: Implantation of perforated punctual plugs is a safe & efficient treatment modality with good tolerance & functional outcome in cases of punctal stenosis with ocular allergy.
Keywords: Epiphora, Punctal stenosis, Perforated plug
Introduction
Punctum stenosis is one of the frequent causes of epiphora besides canalicular or nasolacrimal duct obstruction. It can be congenital or acquired. Acquired punctum stenosis may result from inflammatory or infectious eye disease,chronic ocular allergies, systemic or topical drug toxicity, lid malposition, different forms of trauma, tumours or ageing changes. Associated canalicular and nasolacrimal sac or duct stenosis or obstruction might be present in some cases.1–7. Pure punctum stenosis treatment relies on punctum dilatation, surgical opening or punctum stenting with canalicular tubes or punctum plugs.5,6,8–12
The purpose of this study was to investigate the clinical outcomes and tolerances of polyvinylpyrrolidone (PVP) coated perforated punctum plugs (PPP) in cases of acquired punctal stenosis due to ocular allergy.
Materials and methods
11 eyes of 7 patients with acquired punctal stenosis who received perforated punctal plug implants were included in the study.
Proper informed consent for both the treatment and participation in the study was obtained from the patients.
Inclusion criteria: Patients with acquired causes of punctal stenosis due to ocular allergy
Patients with lid malposition, canalicular or nasolacrimal sac or duct obstruction, previous eyelid or lacrimal drainage surgery, untreated conjunctivitis or blepharitis were excluded.
Diagnosis was based in order on a history of tearing, biomicroscopic examination, fluorescein dye disappearance test, punctal dilatation and diagnostic canaliculi probing, nasolacrimal duct irrigation and if passage is patent after irrigation fluorescein dye disappearance test repetition. Epiphora was scored using the combination of Munk scoreand epiphora scoring of Malet et al (Table 1).

Table 1: Score scale of epiphora
In biomicroscopic examination tear meniscus, lid margin, conjunctiva and punctal orifice was assessed.
[Punctal orifice was graded based on biomicroscopic examination which was examined before punctal dilatation] (Table 2).

Table 2: Grading of punctal orifice.
After biomicroscopic examination, fluorescein dye disappearance test was performed using 1%sterile fluorescein strip and assessment after 3 and 5 min of the remaining dye in the tear meniscus. All patients in the study had over 5 min dye disappearance time. Fluorescein dye disappearance test was graded (Table 3).

Table 3: Grading of fluorescein dye disappearance test.
Procedure : Punctal dilatation, canaliculi probing and nasolacrimal duct irrigation were performed in the operating room under surgical microscope. After instillation of a topical anaesthetic drop (proparacaine hydrochloride ophthalmic solution), a punctal finder was used to open the papilla and pushed forward to dilate the lower punctum. Afterwards a canaliculi probe was introduced. A soft stop that could not be overcome was defined as canalicular obstruction. A soft stop that could be overcome was defined as canalicular membranous stenosis. A hard stop was defined as patent upper canalicular system. Irrigation was performed with a 5 ml syringe filled with serum saline and a 26 gauge lacrimal cannula through the lower punctum and canaliculi. A normal system was defined as free passage of saline into nose or nasopharynx without any reflux through the upper or lower punctum. Patients with any associated canalicular or nasolacrimal duct pathology were not included in the study.
Fluorescein dye disappearance test was repeated after punctum dilatation and found to be under 3 min (grade 1 or 2) in all patients.
After punctum dilatation PVP coated Perforated Punctal Plug implantation was performed.
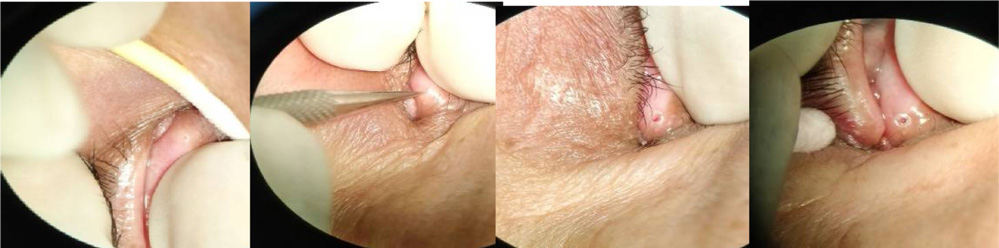
Figure 1: Showing intraoperative steps; stenosed punctum dilated using punctual dilator and perforated punctual plug implanted.
Demographic data, laterality, symptoms, findings of biomicroscopic examination and diagnostic probing and irrigation were recorded. Findings of biomicroscopic examination, fluorescein dye disappearance test and plug tolerance were investigated at postoperative 1st day, 1st month, 3rd month, 6th month(Table 4).Plugs were explanted after 6 months

Table 4: Plug tolerance of patients.
Results
-The age of the patients ranged between 58 and 74 years (mean age 66 years).
-Five (71.42%) patients were female and 2 (28.57%) were male.
-The right lower punctum was involved in 6 (85.71%) patients, the left lower punctum was involved in 5 (71.4%) patients and bilateral lower punctum was involved in 4 (57.14%) patients.
-Upper punctum was involved in 1 eye (9.09%).
-In preoperative examination, 3 eyes (27.27%) had papilla covered with a membrane (grade 1) (Fig. 1), and 8 (72.72%) eyes had punctum less than normal size (grade 2). All eyes had moderate (grade 2, n:2) or permanent (grade 3, n:9) epiphora. Fluorescein dye disappearance test was over 5 min (grade 3) in all patients.
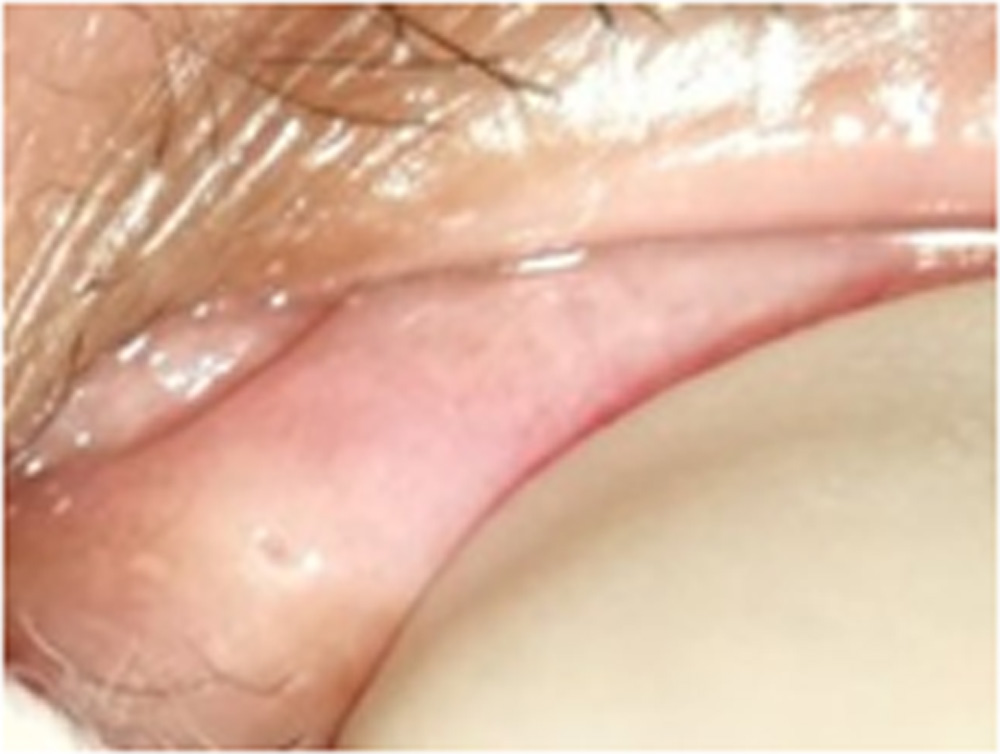
Figure 2:Punctum stenosis grade 1 (punctum covered with a membrane).
-Surgical procedure: After punctal dilatation, control irrigation was performed. Plugs were implanted with their own preloaded inserter after puncti were dilated with the inserters’ own dilatator. In Fig. 2 the punctum with an implanted perforated punctal plug is seen.
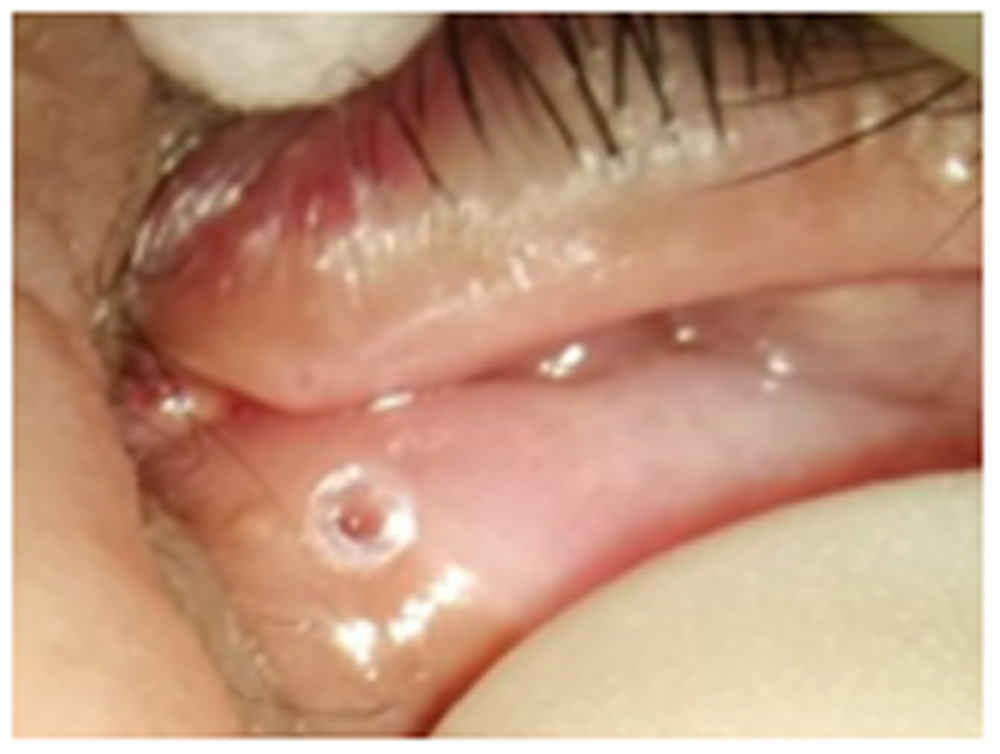
Figure 3:Appearance of an implanted PVP coated perforated punctal plug [comparing with the upper punctum]
-Upper punctal dilatation was performed besides punctal plug implantation in patients having also upper punctum involvement. In one eye the perforated punctual plug implantation was combined with a 3 snip procedure in view of completely stenosed lower punctum.
–Epiphora
The epiphora score was grade 0 in 6 eyes(54.54%) and grade 1 in 4 eyes (36.36%) at 1st day postoperatively. At the end of 6 months 9 eyes had grade 0 epiphora (81.81%) and 2 eyes (18.18%) had grade 1 epiphora.
-Fluorescein dye disappearance test
It was under 5 min (grade 1 or 2) in all 11 eyes after plug implantation day 1 and improved in all eyes at 1st and 3rd month visits [grade 1 in 10 eyes (90.90%), grade 2 in 1 eye (09.09 %)]. Fluorescein dye disappearance test was under 3 min in all eyes after plug explantation at the end of 6 months except 1 eye whose plug dropped off spontaneously in the second month.
-Plug tolerance
Plug tolerance was found good in 63.63% (n = 7) of the eyes at 1st day postoperatively and remained the same at 1st week, and improved to 81.81% (n = 42) at the 1st month visit. Early plug drop off occured in 1 patient (within 3 months). No other serious complications were observed related to the plug.
All eyes were followed upto 6 months post implantation. Overall symptomatic improvement was seen in 72.727% patients.
Discussion
Epiphora is caused by different levels of obstruction in the lacrimal drainage system. In the first step, it is important to distinguish epiphora from lacrimation. Any ocular surface pathology causing lacrimation should be eliminated. If it is epiphora, it is very important to determine the obstruction level of the lacrimal drainage system.
Punctal stenosis is one of the frequent causes of epiphora. Biomicroscopic examination is important in a patient with tearing. Besides ocular surface examination, the aspect of the punctum should be determined. If punctum dilatation and irrigation are performed without biomicroscopic examination or only dacryoscintigraphy is performed without any other diagnostic tests used for lacrimal system, the diagnosis might be mistaken. In this view, to diagnose pure punctal stenosis we performed a fluorescein dye disappearance test, punctum dilatation,diagnostic canaliculi probing and nasolacrimal duct irrigation. If passage was patent after irrigation, fluorescein dye disappearance test repetition.
The punctal orifice is normally 0.3 mm in diameter.5,10 We graded the punctal orifices from 0 to 3 according to the aspect and size of the punctal opening.1 In our study, 27.27% of the eyes had papilla covered with a membrane preoperatively (grade 1) and 72.72% eyes had punctum less than normal size (grade 2). Kashkouli et al. found grade 1 punctal opening rate 86% and 57% in eyes with more than and less than 6 months duration of symptoms, respectively.
Female patients were significantly (71.42%) more in our study which is compatible with the literature. Postmenopausal hormonal changes may be the reason for this sex difference.1,10,14
There are various methods to treat punctal stenosis which are repeated dilatations (generally ineffective); surgical opening with one snip, two snips, three snips or punch punctoplasty; microsurgical punctoplasty with sutures; balloon dilatation; electrocautery; laser treatment or temporary stenting (canalicular tubing, punctal plugs). Despite the high success rate, microsurgery sections the fibrous ring of the punctum, with the subsequent risk of stricturotomy if bicanalicular intubation is later required.5,6,9,10,15
Perforated punctal plugs were first introduced by Bernard et al. to obtain an artificial punctum. The first ones were made of silicone but were not coated with hydrophilic polyvinylpyrrolidone, therefore secretions were obstructing the central orifice. For this reason, the FCI laboratories along with the Le Mans Centre for Technology Transfer modified the hydrophobic nature of plugs, making their surface hydrophilic by coating the silicone plugs with polyvinylpyrrolidone.9,12 In this study PVP coated PPP were used.
Our results showed improvement in the epiphora and the fluorescein dye disappearance test. All eyes had grade 2 or 3 epiphora before plug implantation, and 81.81% of the eyes had grade 0 or 1 epiphora after 6 months following plug implantation.
Fluorescein dye disappearance test score was directly proportional to epiphora score which was grade 1 or 2 in 100% at 1st month postoperatively and decreased to 90.90 % after 6 months follow-up.
Two of the puncti became stenotic again during the follow-up period. The possible explanation for this drawback might be the ongoing of ageing changes, as most of these patients were over 60 years old.9
We left the plugs for 6 months in all of our patients and 2 of them became stenotic again at the end of 6 months. Leaving the plug longer might be more effective.
The advantages of the perforated punctal plugs over surgery are that lacrimal sphincter is not disturbed and it is a less invasive procedure. However there are several complications of punctal plugs including pyogenic granuloma, expulsion, migration, local irritation and the possibility of punctal laceration during insertion.9,13,16–22
Plug tolerance was good in 81.81% of our patients during the 1 and 6 months follow-up.
The complications were early spontaneous plug drop-off in 1 patient. Spontaneous plug loss was reported in 4 eyes in the study by Chung.17 In the study by Malet et al. they compared the tolerance of silicone and PVP coated silicone perforated plugs. They found PVP coated plugs superior to silicone plugs as plug tolerance was good in 75% of eyes and mild in 25% of eyes with PVP coated plugs, and it was only mild in 75% and poor in 25% of eyes with silicone plugs.9
Conclusion
Punctal stenosis is one of the several disorders that cause lacrimal drainage obstruction. Punctal stenosis without any additional ocular surface and lid problems or nasolacrimal system stenosis can be easily treated with PVP coated Perforated Punctal Plugs. Although restenosis may develop in elderly patients, in long term it is a tolerable and effective procedure for isolated punctal stenosis with fairly good response in those with stenosis due to chronic ocular allergy.
Conflict of interest
The authors declared that there is no conflict of interest
References
- Kashkouli B.M., Beigi B., Murthy R., Astbury N. Acquired external punctal stenosis: Etiology and associated findings. Am J Ophthalmol. 2003;136:1079–1084. [PubMed]
- Hurwitz J.J. Disease of the punctum. In: Hurwitz J.J., editor. The lacrimal system. Lippincott-Raven Press; Philadelphia: 1996. pp. 149–153.
- O’Donnell F.E. Medial ectropion: association with lower lacrimal obstruction and combined management. Ophthalm Surg. 1986;17:573–576. [PubMed]
- Seiff S.R., Shorr N., Adams T. Surgical treatment of punctal-canalicular fibrosis from 5-fluorouacil therapy. Cancer. 1985;56:2148–2149. [PubMed]
- Soiberman U., Kakizaki H., Selva D., Leibovitch I. Punctal stenosis: definition, diagnosis and treatment. Clin Ophthalmol. 2012;6:1011–1018. [PubMed]
- Kashkouli B.M., Pacdel F., Kiavash V. Assessment and management of proximal and incomplete symptomatic obstruction of the lacrimal drainage system. Mid East Afr J Ophthalmol. 2012;19:60–69.[PMC free article] [PubMed]
- Ali M.J., Mishra D.K., Baig F., Lakshman M., Naik M.N. Punctal stenosis: histopathology, immunology, and electron microscopic features – a step toward unraveling the mysterious etiopathogenesis. Ophthal Plast Reconstr Surg. 2014 [June 2 (Epub)] [PubMed]
- Kristan R.W., Branch L. Treatment of lacrimal punctal stenosis with one-snip canaliculotomy and temporary punctal plugs. Arch Ophthalmol. 1988;106:878–879. [PubMed]
- Malet T., Challier B., David N., Bertrand A., George J.L. Clinical and scintigraphic comparison of silicone and polyvinylpyrrolidone coated silicone perforated plugs. Br J Ophthalmol. 1998;82:1416–1419.[PubMed]
- Offutt W.N., Cowen D.E. Stenotic puncta: microsurgical puctoplasty. Ophthalmic Plast Reconstr Surg. 1993;3:201–205. [PubMed]
- Edelstein J., Reiss G. The wedge punctoplasty for treatment of punctal stenosis. Ophthalmic Surg. 1992;12:818–821. [PubMed]
- Bernard J.A., Fayet B., Pouliquen Y. Nouveaux modeles de clous meatiques et de pose-clous. Bull Soc Ophthalmol FR. 1989;89:1131–1132. [PubMed]
- Munk P.L., Lin D.T., Morris D.C. Epihora: treatment by means of dacryocystoplasty with balloon dilatation of the nasolacrimal drainage apparatus. Radiology. 1990;177:687–690. [PubMed]
- Hurwitz J.J. Disease of the punctum. In: Hurwitz J.J., editor. The lacrimal system. Lippincott-Raven Press; Philadelphia: 1996. pp. 139–141.
- Jeanolas D., George J.L., Lesure P., Heymann V. Microsurgical treatment of narrow lacrimal points. Bull Soc Ophthalmol Fr. 1987;87:159–161. [PubMed]
- Konuk O., Urgancioglu B., Unal M. Long-term success rate of perforated punctal plugs in the management of acquired punctal stenosis. Ophthal Plast Reconstr Surg. 2008;24:399–402. [PubMed]
- Chang M., Ahn S.E., Baek S. The effect of perforated punctal plugs in the management of acquired punctal stenosis. J Craniofac Surg. 2013;24:1628–1630. [PubMed]
- Bohlman H. Perforated punctal plug in the treatment of partial punctal stenosis. Optometry. 2003;74:524–528. [PubMed]
- Hsu H.S. Ampullary pyogenic granuloma as a complication of lacrimal plug migration. Chang Gung Med J. 2002;25:415–418. [PubMed]
- Bukhari A.A. Management options of acquired punctal stenosis. Saudi Med J. 2013;34:785–792.[PubMed]
- Fayet B., Benabderrazik S., Bernard J.A., Deligne L., Hürbli T., D’Hermies F. Sténoses canaliculaires compliquant la pose de bouchons lacrymaux. Incidence et mécanismes. J Fr Ophtalmol. 1992;15:25–33.[PubMed]
- Kim B.M., Osmanovic S.S., Edward D.P. Pyogenic granulomas after silicone punctal plugs: a clinical and histopathologic study. Am J Ophthalmol. 2005;139:678–684. [PubMed]


Leave a Comment