Dr. Rakesh Juneja, J15026, Dr. Ashish Jain, Dr. Navneet Mehrotra, Dr. Manish Nagpal
Abstract:
Aim: To evaluate the structural and functional correlation in patients with
CNVM (Choroidal Neovascular Membrane) pre & post treatment using MP (Microperimetry)& OCTA (Optical coherence tomography angiography)
Settings and Design: Single-center, prospective, observational study
Methods and Material:56 eyes of 44 patients,treated with intravitreal anti-vascular endothelial factor (VEGF) injections, underwent baseline OCTA, MP & multi-modal imaging. All cases were followed up at 1, 3 & 6 months
Statistical analysis used: Descriptive analysis
Results:OCTA in pre-treatment phase revealed CNVM as an abnormal vascular network arising from the choroid and invading the sub-retinal space. On MP decreased retinal sensitivity was observed corresponding to area of CNVM. Post treatment, OCTA revealed resolution of abnormal vascular network that correlated with increased retinal sensitivity at the corresponding area in MP
Conclusion: Combining the findings of OCTA and MP gives us precise structural and functional changes in response to treatment carried out in CNVMs
Keywords: choroidal neovascular membrane, optical coherence tomography angiography, microperimetry, retinal sensitivity, neovascular network
Key Messages:OCTA-MP correlation is a promising “non-invasive” tool that can be used as an “alternative” diagnostic test and is certainly the ‘future of CNVM imaging’ that bridges the gap between structure and function
Introduction:
CNVM results in photoreceptor damage and vision loss. [1, 2]Fluorescein angiography (FA) still remains the gold standard. [3]However, being invasive it carries certain risks.[4, 5]
Optical coherence tomography angiography (OCTA) allows visualization of retinal and choroidal vasculature non-invasively. [6]Microperimetry (MP) is used to evaluate macular function by measuring retinal sensitivity. [7, 8]
The aim of the study was to correlate the functional treatment response using MP (MP-3; Nidek, Gamagory, Japan) with the morphological findings on OCTA (AngioScan OCT Angiography software on the RS-3000 Advance Nidek) by structure-function correlation in choroidal neovascular membrane (CNVM) secondary to AMD.
Subjects and Methods:
Study design and patient enrolment:
This was a single-center, prospective, observational study. Institutional Review Board after studying protocol provided approval for the study. All cases provided informed consent to be enrolled in the study. Data was collected from patients diagnosed as Age Related CNVM at retina clinic.
Eligibility criteria and data collection:
Data was collected under the following headings: demographic details, history of presenting illness, eye laterality, history of associated systemic co-morbidities, clinical examination details including visual acuity at presentation and follow- up with multimodal imaging features, treatment details, complications (if any) and treatment given for that complication. Inclusion criteria were: (1) Age >50 years (2) clinical findings consistent with active stage of Age Related CNVM pre-treatment at presentation (3) follow-up of at least 6 months and (4) complete availability of documentation till the last follow-up. If any one of the above-mentioned inclusion criteria was not met, patients were excluded from the study.
Investigations:
Diagnosis of age related CNVM, was made by clinical and relevant imaging tests like OCT and FFA at presentation.
Treatment Regime:
All patients were treated with 3 injections of intra-vitreal anti-VEGF at monthly interval for 3 months. All patients were followed at 1, 2, 3 and 6 months (from baseline).
Study Parameters:
Patients who met inclusion criteria were enrolled in the study. All cases at presentation (i.e. before 1st injection) and during1st (prior to 2nd injection), 2nd (prior to 3rd injection), 3rd (1 month after 3rd injection) and 4th (3 months after 3rd injection) follow-up, underwent complete eye examination. The examination protocol included best-corrected visual acuity (BCVA) with the help of Snellen’s Chart, and converted to logMAR (logarithm of the minimum angle of resolution), dilated fundoscopic examination, color fundus images (Topcon 50 Dx, Medical Systems Inc, Oakland, NJ, USA), spectral domain-optical coherence tomography (SD-OCT) (Spectralis, Heidelberg Engineering Inc, Heidelberg, Germany). OCTA centered on the fovea covering 3×3 mm area (10° x 10° field of view), MP-3 centered on fovea covering 45° field of view.
Data Analysis:
Using ‘overlay’ feature, morphologic characteristics of OCTA at the site of CNVM lesion were analyzed& correlated functionally with MP-3.
Results:
Baseline Demographics:
Eighty-six eyes of 48 patients were studied. Out of these, 56 eyes of 44 patients met our inclusion criteria and were enrolled in the study for further analysis. The mean age at presentation was 57.8±11.6 years. Thirty-two eyes had unilateral presentation. The gender distribution comprised, 34 eyes of male and 22 eyes of females. All subjects included in the study were Asian Indians. (Table 1)
Correlation of OCTA and MP features of CNVM:
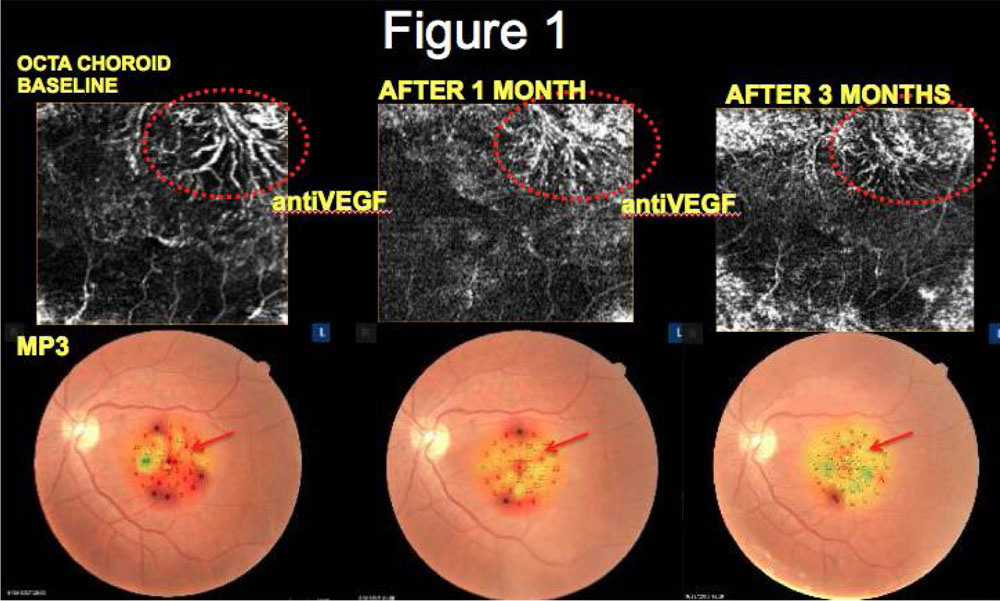
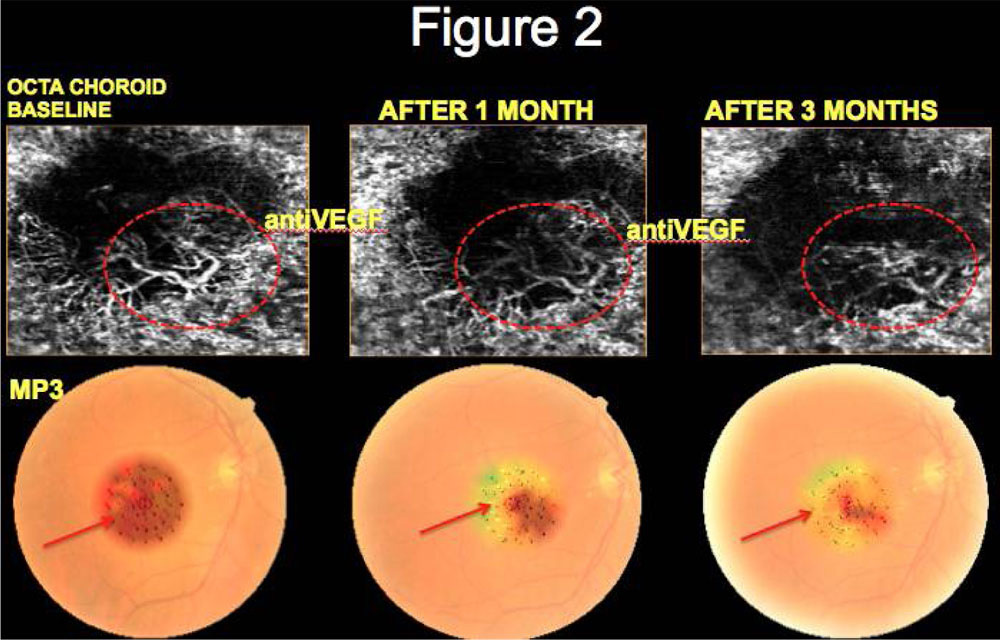
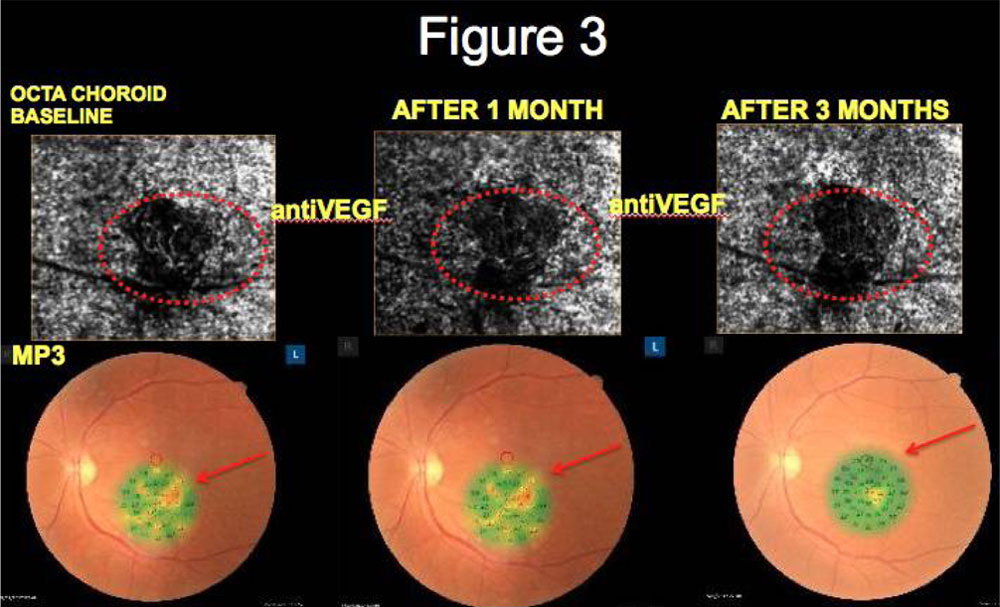
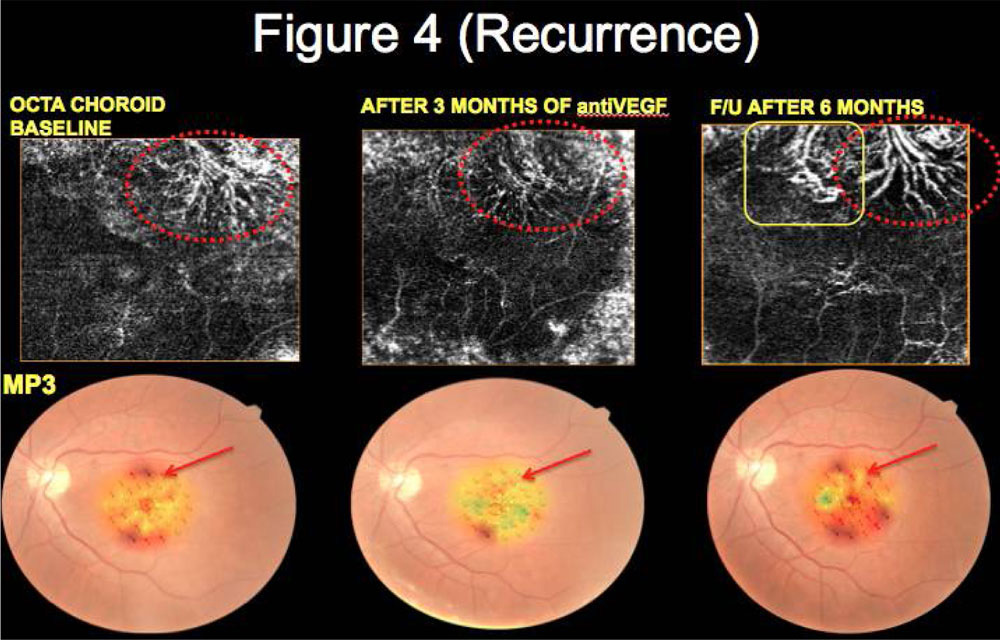
OCTA in pre-treatment phase revealed CNVM as an abnormal vascular network arising from the choroid and invading the sub-retinal space. On MP3 decreased retinal sensitivity was observed corresponding to area of CNVM. Post treatment, OCTA revealed reduction of abnormal vascular network in 51 (91.07%) eyes that correlated with increased retinal sensitivity at the corresponding area in MP3 for all 51 eyes. (Table 2) (Figure 1, 2, 3, 4)
Discussion:
In this study we have made an attempt to correlate the structural data provided by OCTA with the functional information obtained by MP-3 using a novel ‘overlay’ software for the first time. There was a significant correlation observed between the neovascular network on OCTA with decreased retinal sensitivity on MP-3. Post treatment with resolution of neovascular network on OCTA, a significant improvement in retinal sensitivity was documented on MP-3. Various studies in literature have made an attempt to correlate the structural and functional information in cases of age related CNVM by using SD-OCT and MP-1 [7, 8, 9].
MP-3 introduced in 2015, offers certain advantages over MP-1 in terms of luminance and ability to measure a wider retinal sensitivity threshold deploying less energy in a quick time. OCTA on the other hand is the only non-invasive tool that provides 3-D analysis of CNVM and provides structural information of neovascular network. Overlaying the details of OCTA and MP-3 with the help of novel software provided by Nidek provides us a new insight to the understanding of disease process that was never explored previously.
Other methods of assessing the functional outcome at baseline and in response to treatment with various available modalities are measurement of best-corrected visual acuity, which gives a crude assessment. MP-3 helps to overcome this significant dis-advantage and provides much more refined and point-to-point information at each and every visit in context to the underlying pathology. Even in cases of good visual acuity with early juxta-foveal CNVM, MP-3 detects the presence of decreased retinal sensitivity.
Our study has few limitations as small number of cohorts, lack of further long-term follow-up beyond 6 months and non-availability of swept-source OCTA that can further provide more insight in context to morphological changes. MP-3 also needs a long-term validation on the basis of clinical trials and including other pathologies as well before it can be quoted as confirmed method of analyzing the structure-functional correlation.
Nonetheless to conclude, the novel ‘overlay’ software provided by Nidek is a promising imaging tool. Combining the findings of OCTA and MP3 using ‘overlay’ feature gives us precise information of structure-function correlation at presentation & also in response to treatment. More importantly it helps to improve patient’s compliance, confidence to treatment and their understanding of the disease process as well. It also serves as a means of visual rehabilitation in visually handicapped cases and bridges the gap between morphology and function accurately.
Abbreviations:
OCT optical coherence tomography
CNVM choroidal neovascular membrane
MP Microperimetry
OCTA optical coherence tomography angiography
References:
[1] F. L. Ferris III, S. L. Fine, and L. Hyman, “Age-related macular degeneration and blindness due to neovascular maculopathy,” Archives of Ophthalmology, vol. 102, no. 11, pp. 1640–1642, 1984.
[2] J. Ambati, B. K. Ambati, S. H. Yoo, S. Ianchulev, and A. P. Adamis, “Age-related macular degeneration: etiology, patho- genesis, and therapeutic strategies,” Survey of Ophthalmology, vol. 48, no. 3, pp. 257–293, 2003.
[3] D. V. Do, “Detection of new-onset choroidal neovasculariza- tion,” Current Opinion in Ophthalmology, vol. 24, no. 3, pp. 224– 227, 2013.
[4] P. E. Stanga, J. I. Lim, and P. Hamilton, “Indocyanine green angiography in chorioretinal diseases: indications and interpre- tation: an evidence-based update,” Ophthalmology, vol. 110, no. 1, pp. 15–50, 2003.
[5] M. P. Lo ́pez-Sa ́ez, E. Ordoqui, P. Tornero et al., “Fluorescein- induced allergic reaction,” Annals of Allergy, Asthma and Immunology, vol. 81, no. 5 I, pp. 428–430, 1998.
[6] A. Nagiel, S. R. Sadda, and D. Sarraf, “A promising future for optical coherence tomography angiography,” JAMA Ophthalmology, vol. 133, no. 6, pp. 629–630, 2015.
[7] Steinberg JS, Saßmannshausen M, Pfau M, Fleckenstein M, Finger RP, Holz FG, Schmitz-Valckenberg S. Evaluation of Two Systems for Fundus-Controlled Scotopic and Mesopic Perimetry in Eye with Age-Related Macular Degeneration. Transl Vis Sci Technol. 2017 Jul 13;6(4):7.
[8] Sulzbacher F, Roberts P, Munk MR, Kaider A, Kroh ME, Sacu S, Schmidt-Erfurth U; Vienna Eye Study Center. Relationship of retinal morphology and retinal sensitivity in the treatment of neovascular age-related macular degeneration using aflibercept. Invest Ophthalmol Vis Sci. 2014 Dec 11;56(2):1158-67.
[9] Midena E, Vujosevic S, Convento E, Manfre’ A, Cavarzeran F, Pilotto E. Microperimetry and fundus autofluorescence in patients with early age-related macular degeneration. Br J Ophthalmol. 2007 Nov;91(11):1499-503
Table no. 1: Baseline Demographics
| PARAMETERS | n (%) |
| No. of patients | 44 |
| No. of eyes | 56 |
| Male | 34 (60.71) |
| Female | 22 (39.29) |
| Age (mean) | 67.54 |
| Age (range) | 55-85 |
| Unilateral | 32 |
| Bilateral | 12 |
Table no 2:Correlation of OCTA and MP features at baseline and follow-up visits
| NUMBER OF EYES | VISITS | OCTA FEATURES | CORRESPONDING MP FEATURES
(on the same location) |
|
51 |
Baseline
(prior to 1st injection) |
Abnormal neovascular network encroaching sub-retinal space from choroid
|
Decreased retinal sensitivity |
| 1st follow up
(prior to 2nd injection) |
Decrease in size of neovascular network
|
Slightly improved retinal sensitivity | |
| 2nd follow up
(prior to 3rd injection) |
Further decrease in size of neovascular network
|
Further improvement in retinal
sensitivity |
|
| 3rd follow up (3 months after 1st injection)
|
Significant resolution/decrease of neovascular network
|
Increased retinal sensitivity | |
| 4th follow up (6 months after 1st injection) | Near total resolution of neovascular network
|
Increased and stabilised retinal sensitivity |
Figures: Correlation of OCTA and MP features of CNVM at baseline and follow-up
Figure 1:
Figure 2:
Figure 3:
Figure 4:






Leave a Comment